Too Long; Didn’t Read (TL;DR)
My new hip is amazing and before long I’ll be moving like it’s brand new.
My hips are congenitally shit, really, my whole lower spine including pelvis, and this is not the first time it’s all been a bit problematic. But this is the first time I’ve had a total joint replacement of the hip! There was some minor if mess-making excitement in the recovery room but it’s all fine. Now I have new hip hardware like some kinda Junior League Terminator, and almost four weeks post-surgery - when I was taken care of fantastically by the team at Kaiser, San Jose - I’m walking w/o a cane, all my various stages of bandages are removed, and I’m off all the post surgery meds except a little blood-thinning aspirin to prevent clots, through the end of the month.
For a longer version, read on!
(Yes, there are pictures. Don’t worry, I put them at the bottom under some reveal checkboxes. You’ll never see them if you don’t want to!)
First, the Ow!
For most of my life, there have been some indications of what I’ve heard referred to in others as “skeletal disharmony”. I had some weird numbness in my lower body as a kid, and also it turns out there is a history of relatively early hip replacements in the men in my mother’s paternal line.
Perhaps related, my back has hurt for years. I always attributed it to too much martial arts and too much hockey, both fun things I did for years that are hard on your body. In more recent days, my left hip was grinding with every motion; walking, standing, sitting. And I wasn’t doing any running or deadlifts anymore, I tell you what.
But I first knew something was wrong with my left hip in 2015 or so. One day I went for a run, got about six steps into it, and there was a most disquieting snapping sensation deep in the joint accompanied by a stabbing pain. Ow!
I stopped for a moment to gingerly test it out, and it definitely didn’t feel right; the range of motion was limited, the whole thing felt suddenly swollen in a way it hadn’t moments before. I lowered my ambition in terms of stride, but set out again. I didn’t make it very far before I stopped and limped the half-block back home.
For the next couple of years, sometimes I could get in a run, or a set of deadlifts, and sometimes I could not, often accompanied by some similarly disquieting internal event. The frequency of “not” continued to increase along with the discomfort during those times. It was then time to get a medical opinion.
That ain’t right, but it ain’t broke
In 2017 I got a referral to imaging and a specialist’s analysis. Clear on the imaging of my pelvis and back were a couple of things;
- My lumbar vertebrae were sliding backwards out of place . Just a little. This is why my back hurts all the time.
- There’s arthritis in both hips along with decay of the cartilage.
The takeaway was that:
- There’s not a lot to do for the back. Some chronic pain medication and some specific daily exercises would probably help (they did). Nowhere near needing surgery and the surgery results kinda suck, so avoid it (I like being able to twist at the waist).
- The hip decay “wasn’t even moderate” and surgery wasn’t indicated, yet. Some chronic pain medication and some specific daily exercises would probably help (they did).
A few years later…
So while the medications and the exercises helped A Lot at first, there were diminishing returns over time. Eventually, doing the exercises at all was causing me pain, so I stopped doing them. I was in literal constant pain at this point. It hurt when I was sleeping (it’d wake me up), it was a bone-on-bone grind when I was walking, sitting down, standing up, or even shifting my seated weight.
It was time to escalate.
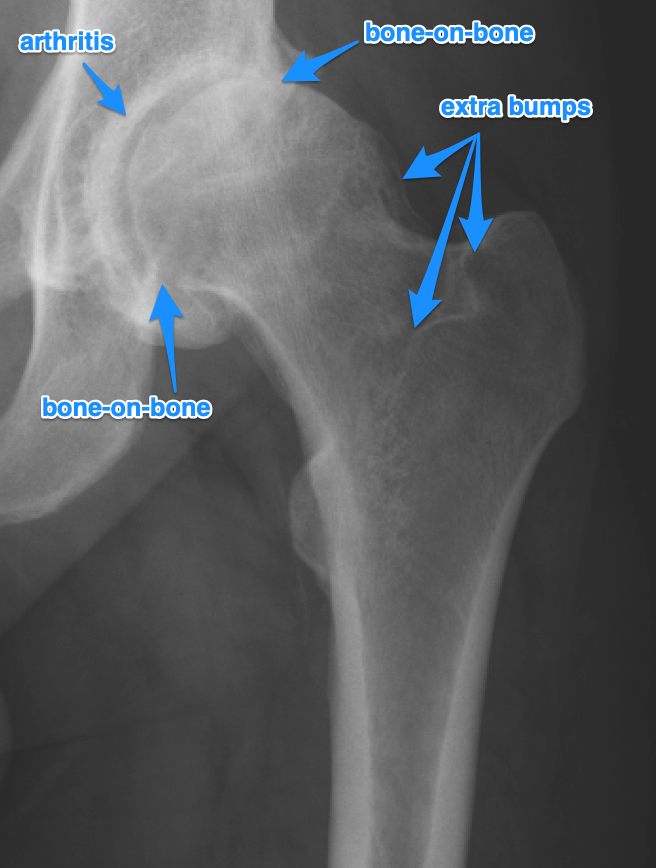
I contacted my primary physician, but they were not much interested in sending me on to imaging and specialists. So I changed primary physicians. This is a thing you can do and I recommend you do it as needful. New primary sent me straight on to imaging. You can see that X-ray below (only if you want, it’s hidden) and I’ve marked it up with what was pointed out to me.
The tl;dr is that the factory part was worn out and it was time for a replacement. Woohoo! This is the result I was hoping for.
Getting into surgery
Now, you’ll note that this is happening as the same time there is a global pandemic that is driving unusual hospital practices like cancelling elective surgeries like mine.
[aside: This surgery doesn’t feel very elective. I know that’s the phrase used when the surgery isn’t life-threatening. Personally, I think we should expect “necessary” to include quality of life-threatening, but, welcome to the American health care system 😛]
However, here in California, it seemed like we were stabilizing the outbreak and the hospitals started scheduling some of these elective surgeries again, with added precautions of course, like Plexiglas barriers at counters, mask requirements and lots of hand sanitizer.
As a relatively young person who wasn’t overweight, didn’t smoke or have diabetes, I made a great candidate for surgery during this time. I got moved to the front of the line past the folks more at risk during surgery in the time of the coronavirus SARS-CoV-2. I was scheduled for June 8, 2020.
I did some calling around, talking to family (thanks, Uncle Brian!) and various surgeons before I landed on a surgeon and an approach (“direct anterior” ) I wanted.
The Day Of
First ones, first.
I drew the first slot of the day for my surgeon. I was actually excited by that. Gettin’ them fresh! It did mean I had to get there at 6:45 and be checked in by 7:00. Hey, for this? No problem.
After checkin, I changed into a couple of gowns, had a pee (foreshadowing!), and got under the warm air-inflated blanket on my bed (that thing was awesome) to await the myriad sensors, IVs and medications that were about to begin, including the spinal block that was going to keep me from feeling anything. They were also going to give me something to make me sleep, for my comfort and probably to make sure people don’t freak out during the procedure. Hey, I was happy to miss the middle bits and stay out of the way, so that was fine with me.
The team at Kaiser, San Jose was fantastic. I felt very well taken care of as they got me ready.
At just about 7:30, the surgeon came by for a final chat. His main point was that anyone how makes it this far does great, this surgical team had worked together on 100’s of these and everyone knew what to do, perfectly…
… so long as no one tried to sneak something in like a drug addiction. At this point he fixed me with a penetrating stare.
I simply shook my head gently and replied, “Nope. All good to go. Eager to get started.” [Narrator: In fact, he does not have a drug addiction.]
“Great!” he replied, then off he strode to get ready.
Ten minutes later, they were starting to put me under and wheeling me in.
In the room where it happened
(ObOverusedHamiltonReference) (Lowkey fuck you, John Bolton )
Once in the room I got to experience that thing you see all the time on TV, where like six people count to three and then heave someone over onto the operating table from the gurney. It’s fun! They were super smooth. Also I was pretty stoned by this point and I’m not sure a lot wasn’t fun.
The next super-fun thing they did was strap me into the booties for the Hana table. The what? Oh, just this thing .
See those boot-lookin’ things? Those are boots. They have closures similar to ski boots so of course I made the joke I am sure they have never heard before (in my defense, remember I’m stoned) about how I should have brought my ski boots. I sort of remember them clipping me in, then putting some sort of translucent box shield over me and I’m out.
…for a while. Later, I wake up to the sound of cheerful voices I identify as the doctor, who I can hazily see through the translucent shield, and who I presume is the surgical team. I’m awake because of “the buzzing” and the “tickling”. To myself I think “oh he’s using some router tool on my hip thass cool kk bye now” and then I went back to sleep. You might write this of as me being, well, stoned, but the surgeon was careful to mention in the post-op call to Jamie that I’d woken up and it happens sometimes, it was only for a few seconds, they try really hard to avoid this kind of thing and they’re sure I didn’t feel anything. They were right. I did not feel anything. Well, not much. I woke up because something was tickling my ribs and there was a noise. And it was the vibration of that router tool through my meatsack and of course the sound it makes merrily spinning through bone. Neat!
In Recovery
I don’t really remember coming down the hallway from the OR. I sorrrrrrta remember being awake in the OR after surgery on the Hana table. Then I was back in the bed heading out of the OR, then I was in the recovery room and suddenly awake.
They sit me up and start talking to me and I’m pretty sure I’m talking back to them just like a person who has recently woken up; obviously wide-eyed but obviously not totally all there yet.
This doesn’t last long, and I am presented with a couple of tasks before I can go home:
- Pee
- Navigate the floor and a step up and down using a walker
Peeing is a big deal. You do not get to go home until you pee and you will be right back in the hospital if you stop peeing. Apparently something about how the body reacts to surgery sometimes results in people not peeing after surgery. I, as we are about to learn, am Not That Person.
Running the Walker Course is going to have to wait until my spinal anesthetic wears off, which it has not yet as I can’t really move or feel my legs or toes yet (yep, I was trying with interested curiosity), and hey this is a good time to talk about peeing again.
They brought over an ultrasound wand and handed me an excellently rectangular bottle with a handle on top and the quite-ample opening angled just right. They went to apply the wand with a glib, “oh that IV really packs fluids into let’s see if you have a litter of urine in there yet…” Followed immediately by a startled, “Oh! You are already peeing!”
Remember, friends, that the spinal hasn’t worn off. I can both not feel my very full bladder (a cursory swipe of the ultrasound was annotated with “Oh yes, that’s at least a liter.”), nor the liquid running all over me, nor, as it happens, my weenus itself, but more on that later.
So, what is happening now isn’t really peeing, it’s overpressure not being held back my muscles that are currently on medically-induced recess. Also hampering peeing, is muscles being on medically-induced recess. I’m told that some gravity helps in this situation, after some close interrogation as to how well my legs are working (Some, not A Lot) I’m sat on the edge of the bed with my bottle so they can change some of the bed behind me, and things seem to be going well! I push a little with my non-surgeried leg to keep me on the bed, and I’m leaning my torso back and have my free hand back on the bed a bit for bracing and balance.
This is when I get worried if I’m actually peeing in the bottle. As you’ll recall, I can’t feel it. I don’t hear liquid hitting the ground, but it’s not exactly quiet in here in this big room full of post-surgery patients and their pained groaning, slap-happy babbling and staff going to and fro with all their duties and nothing but concrete and thin curtains to contain the sound.
So I bend down a little to look. Yes! Weenus is safely in the bottle! This is going great. I’ll lean back now. Uh. I’m not leaning back. Engaging some More Effort, I try that again. Nope. In fact, sort of going the other way now.
“Damnit,” I said confidently.
And right then, friends, is when I toppled off of the recovery bed onto the floor, peeing, with a wide-mouthed bottle of pee in my hand.
Some excitement ensued. This was entirely my fault.
For my part, the excitement I was focused on was directing my topple toward my non-surgeried side and making as circular an impact surface as I could (knee -> thigh -> hip -> tuck chin to chest, shoulder -> oof) and I’m pleased to announce that I accomplished that mightily. I was not hurt, at all, in the fall. Not even a later bruise arose. I did bump a supply cart and send it rolling majestically across the ward, but it was likewise not injured.
A mob scene of nursing staff piled on me at this point. Three people almost a foot shorter than me and of considerably less mass and very familiar with handling larger people who don’t entirely have their normal bodily operations on straight. I was scouted for injuries and good sense (weirdly, this is a thing they check when people throw themselves out of bed straight after they’ve had a full joint replacement). I assured them I was fine, and no, not dizzy at all but we’d get back to the good sense thing as I had some self-critique on that, and they pulled me up with some little assistance from myself (at this point I could push pretty well with my legs, but uh, needed directional guidance) and got me back into bed.
They had not changed the bed. I’d sorta interrupted that. But they did put down some pads between me and the considerable amount of pee.
Oh yes. The urine. We’d almost forgotten about that hadn’t we.
Recall, that I was peeing as I was falling and I was holding an open, wide-mouthed bottle of urine. As they put me back into bed I got a glimpse of the floor and what seemed to be a pretty solid impressionistic rendering of the Great Lakes. (Andan Lauber (b. 1973); Lakes, Not So Great, 2020; Urine on tile).
My nurse was Not Best Pleased. “Oh I’m going to have to do so much more paperwork and you’re going to get sooo many visitors. And you broke my perfect No Falls streak.”
“Urm. I’m very sorry. It’s 100% my fault.”
“:glare:”
“I’m really, very, very sorry. …visitors?”
“Yes. Everyone in the chain has to come see you and make sure you are OK, now.”
“Um. Damnit. Sorry. Oh! Did you hear! I said ‘damnit’ when I fell!”
“Yes, I heard. I was very busy not saying a lot more very colorful things.”
“Heh.”
There was good-natured banter through the rest of my stay (“I’m going to go check on that other patient. You. Stay. In. Bed.” “:grin: Where’s the truuuuuuust?!” “Gee, I wonder!” :all laugh:). Honestly, the whole team was great about it all, and I did get a lot of visitors. Several of whom mentioned that I didn’t at all look like I’d just had major surgery (oh buddy, they should have just visited me a few days later. I sure did then).
Sometime later, they came around with the walker to see if I could do the course, but my legs weren’t all awake yet and my blood pressure didn’t do great when I stood up with the walker, bedside. Which I reported! Without doing anything dumb! “I can’t use the backs of my legs or my glutes yet, and also, I feel a little dizzy.”
“Oh yeah, your BP just dropped a good bit. Have a seat, let’s get you back in bed. We’ll try again in an hour or so.”
And so we waited and in the meantime I would probably need to pee again, but this time with Less Excitement, Please. This I accomplished in due course, staying in the bed and actually being able to use bladder-related muscles again. Though… and this was weird… I could see me aiming my weenus into the bottle, but I 100% could not feel my fingers touching it. So now I know what that’s like. My nurse explained that as the spinal wears off, sensation and control comes back vertebrae by vertebrae pretty much, as branch points for the spinal column. Your junk is wired in to L2, so apparently that wasn’t awake yet. I promised to, and did, perform periodic L2 checks.
Nurse: “I am telling Jamie that I did not make the L2 check, you did.”
Me: “Oh, totally! She will believe you.”
She did. And, she did. I’m such a dude in some regards.
Anyway, later, I passed the blood pressure test, and then I crushed the Walker Course.
I left the hospital at about 13:40, being wheeled out to the car where Jamie was waiting to drive me home, and navigating my way into the seat using the door and frame and seat as guides. It wasn’t that bad.
So yeah, you really do stand up within hours of these sorts of surgeries and that’s a thing you can do.
Recovery at home
The first day you feel awesome. Kind of pleasantly tired, very chatty, and just happy to lie on the couch with your foot up and some ice shoved down your pants. It’s great. Days two through five are a bit rougher. The really cool drugs you got at the hospital have worn off and you feel exactly like someone used power tools on you. This is held at some remove by the pretty good drugs they sent home with you, but that stretch is a good few days to sleep a lot.
Home Health comes to visit to change your bandage (everything looks great) and give you some tips on what to look out for (none of which happened) and give you a sense of how how the next few weeks are going to go and make sure you are using your walker right. Later, they help you transition to a cane, and take your staples out.
Along the way, they give you an escalating series of exercises to do. You need to work on your glutei, and there’s a system of muscles down the outside of your leg from hip to ankle that has a) been abused by your compensatory walking habits during the time your hip was degenerating and causing you pain b) pretty worked in the thigh region during your surgery, so don’t strain it too much. Work on those glutei. In week four, I’ll be going back to light duty in the gym; some amiable recumbent bicycle work. Maybe get through some podcasts.
Now, I’m entirely self-mobile and since I’m off the Percocet, I can drive. I don’t drive far but it’s 💯 a thing I can Just Do.
In closing
I don’t have grinding pain every day, all day, anymore. I just just, bend right at the middle and pick stuff up, or check my teeth in the mirror or whatever.
And it’s amazing.
15/10 would do again.
I mean, in a few years, I’m going to have to.
The right hip is on its way out. It’s going to be fine. I won’t wait as long next time.
Images
Because not everyone wants to see these sorts of things, and I respect that, I’ve hidden these images under acknowledgements. Just check the box to reveal the described image.
Pre-surgery HipHere's an X-ray of my hip from a few months before my surgery. I've marked it up with some of the things that were pointed out to me as Not Good.
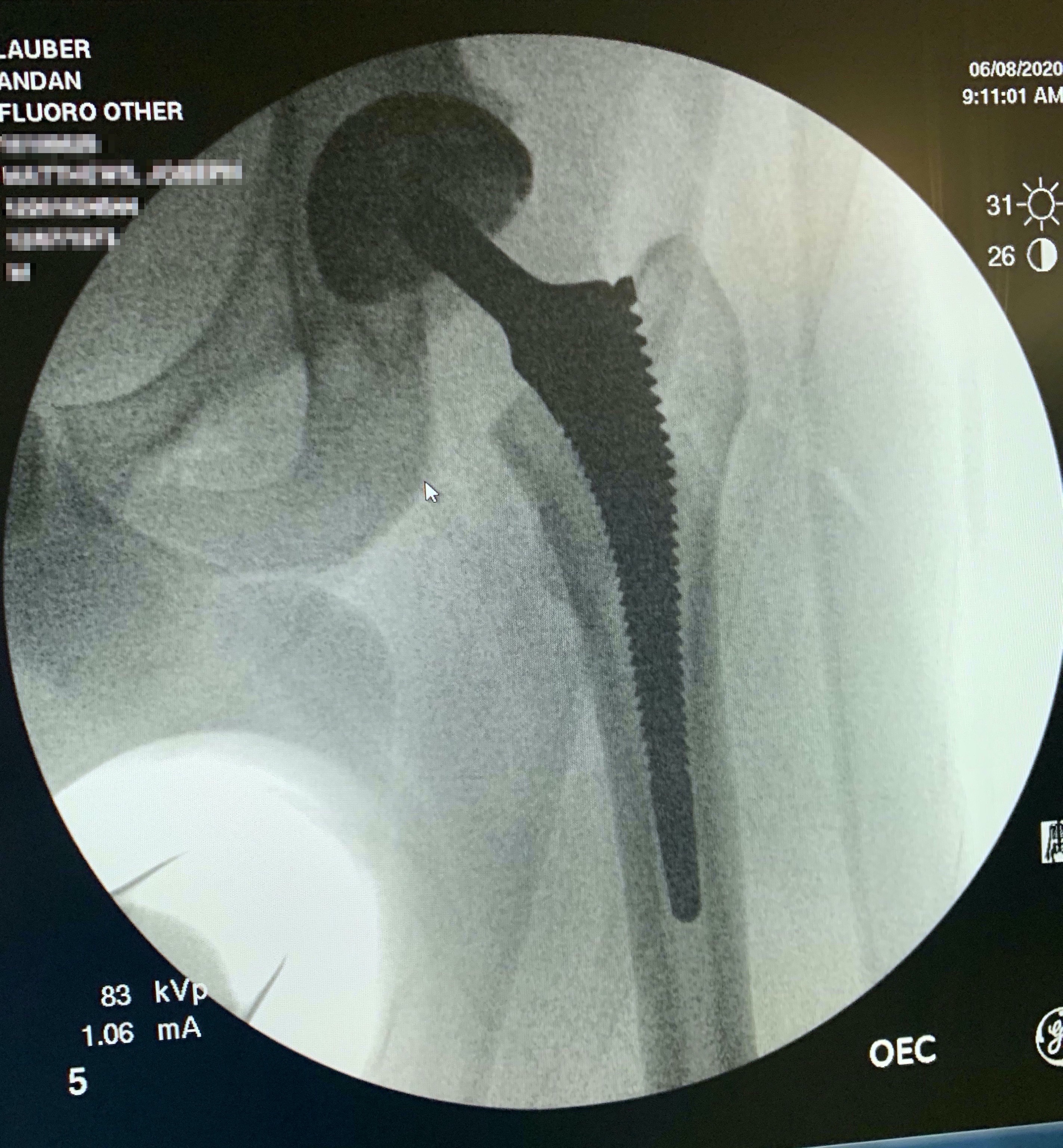
Post-surgery hip
Another X-Ray. Whoa. Gnarly. You can see where the hip socket was routed out, and where the top of the femur including the ball joint was removed. And of course the implant that was hammered into my marrow is hard to miss 😎
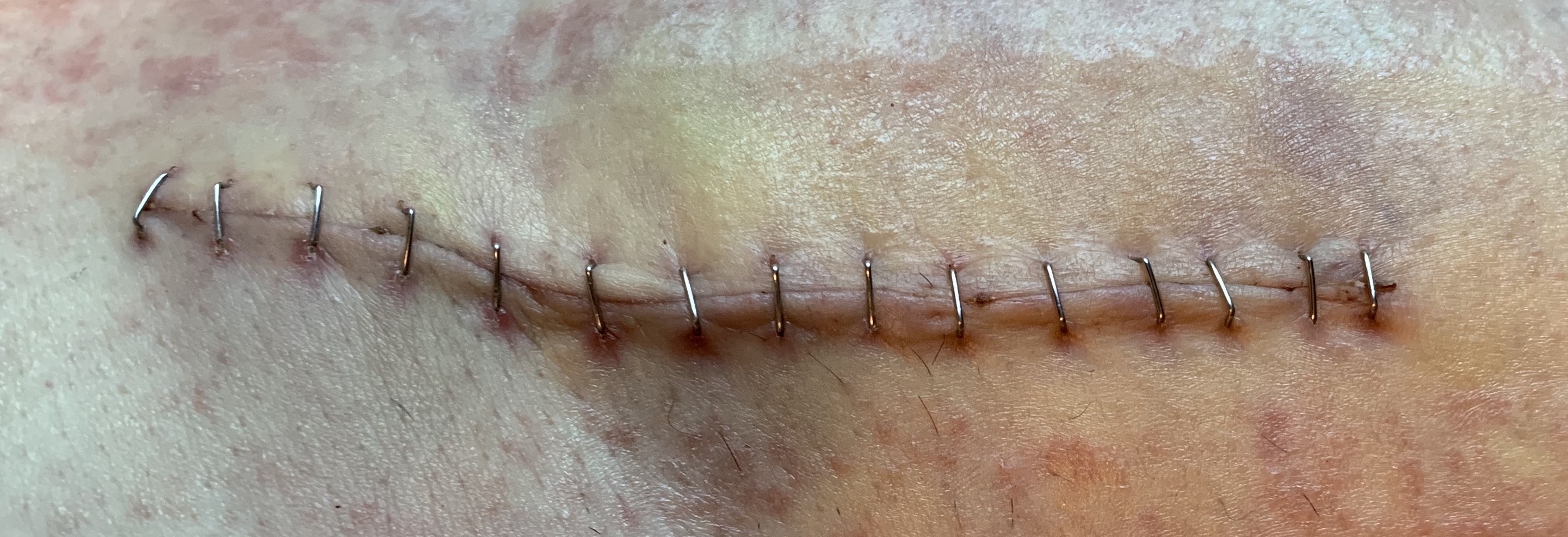
Staples
The incision was closed with staples. I've never had staples before! They are pretty wild. Here there are during the first dressing change, about three days after surgery. The skin is still bruised from being pried out of the way and that rash is from the glue on the bandage. It's pretty intense glue.
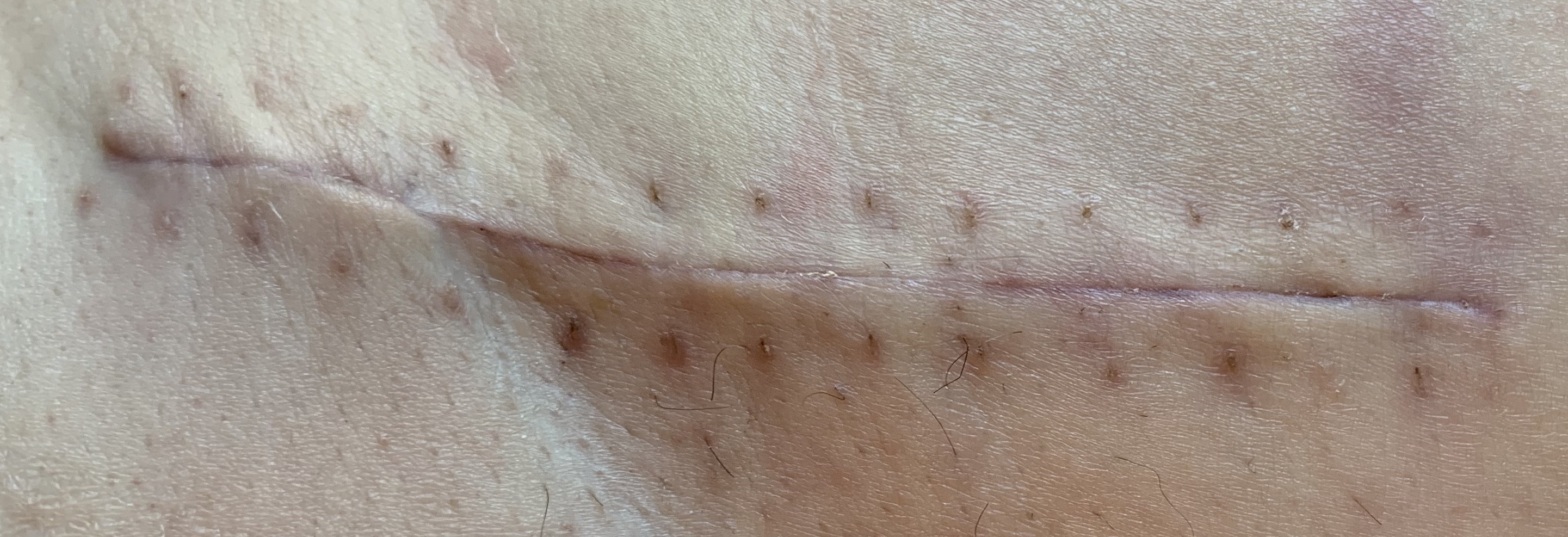
Scar
After the staples came out, which was about two weeks after surgery, you get steri-strips placed across the incision. These last from days to about a week. As of this writing, the last ones fell off yesterday revealing my new scar.